
Sunday, January 31, 2010
Saturday, January 30, 2010
Two for three during the wintry week
Busy, busy week back at work. I got home from NAVC on Thursday afternoon. I finally caved and took a Xanax to fly. I've only ever taken Xanax once in my life, and it was also to fly. Since then, I've been fine on planes. I knew I would be apprehensive about this flight though because of the cloudy, rainy weather. Take-off was nerve-wracking, as always, and I just assumed the tiny dose of Xanax I took didn't work (0.25mg for anyone interested). As it turns out, it must have worked some. I failed to notice that many people on the plane were vomiting due to the turbulence (pointed out to me after landing by my somewhat shaken flight companion). The turbulence itself didn't even phase me. Go figure. Oh, and the fact that our plane taxiied out to the runway, then had to taxi back to the gate for flap repair, and we were delayed over an hour didn't phase me either.
What I left:

So, I got back Thursday night, started back to work Friday night. I've worked the last 6 nights out of 7. It's been hectic. Saturday night, I had a lovely 18 month old Bull mastiff with a fluid distended stomach. I removed a rubber ball from her intestines. The next night, I had a dachshund that liked to eat acorns. I removed that from the small intestines as well. Both patients are doing great at home and I consider them successes to add to my list.
Last night was my final night, and I had another patient with acute vomiting, history of eating multiple foreign bodies, and progressively worsening gastric dilation with fluids on xrays over several hours. The radiologist said point blank, "if this was my dog, I would cut." I felt the same way. You can guess what happened...we cut...and there was nothing. We released the evil spirits and closed the dog back up. I hate, hate, hate, hate, hate doing negative exploratory surgery. Its costs the owners a lot of money, which can be stressful in this economy, it puts the animal at risk for post-operative complications (I had to open the stomach in this case to examine the contents, which turned out to be a lot of kibble, fluid, wood chips, and hair - but no obstruction), and carries the risk of anesthetic death. It's something every vet does and something most vets HATE. I am no exception. So, of course, I go back over the evidence and convince myself I should have known better...and of course, surgery could have waited...and blah blah blah.
I'm off for 4.5 days, and I need it desperately. I'm so tired right now my chest hurts. The weather is FABULOUS for staying indoors. The roads are ice/slush, there is 2-3 inches of white powder in front yard, and I don't have to do anything until Wednesday night. I'm happy. I'm one of those people that still gets giddy like a child when I see snow.
Cardinal sentinel:

Some pictures of the "beautiful" weather we're having, as well as one of the beautiful weather I just left. The bird congegration was taken through the screen porch door so as not to disturb the fluffies. At one point, there were 15+ birds in that tree including 2 female cardinals, 2 male cardinals, a blue jay, a mockingbird, a robin, and a couple I didn't recognize. Oh and a lonely chickadee.
Porch kitty demonstrating her kitty door (and delicate, feline sensibilities about getting her paws damp):





What I left:
So, I got back Thursday night, started back to work Friday night. I've worked the last 6 nights out of 7. It's been hectic. Saturday night, I had a lovely 18 month old Bull mastiff with a fluid distended stomach. I removed a rubber ball from her intestines. The next night, I had a dachshund that liked to eat acorns. I removed that from the small intestines as well. Both patients are doing great at home and I consider them successes to add to my list.
Last night was my final night, and I had another patient with acute vomiting, history of eating multiple foreign bodies, and progressively worsening gastric dilation with fluids on xrays over several hours. The radiologist said point blank, "if this was my dog, I would cut." I felt the same way. You can guess what happened...we cut...and there was nothing. We released the evil spirits and closed the dog back up. I hate, hate, hate, hate, hate doing negative exploratory surgery. Its costs the owners a lot of money, which can be stressful in this economy, it puts the animal at risk for post-operative complications (I had to open the stomach in this case to examine the contents, which turned out to be a lot of kibble, fluid, wood chips, and hair - but no obstruction), and carries the risk of anesthetic death. It's something every vet does and something most vets HATE. I am no exception. So, of course, I go back over the evidence and convince myself I should have known better...and of course, surgery could have waited...and blah blah blah.
I'm off for 4.5 days, and I need it desperately. I'm so tired right now my chest hurts. The weather is FABULOUS for staying indoors. The roads are ice/slush, there is 2-3 inches of white powder in front yard, and I don't have to do anything until Wednesday night. I'm happy. I'm one of those people that still gets giddy like a child when I see snow.
Cardinal sentinel:
Some pictures of the "beautiful" weather we're having, as well as one of the beautiful weather I just left. The bird congegration was taken through the screen porch door so as not to disturb the fluffies. At one point, there were 15+ birds in that tree including 2 female cardinals, 2 male cardinals, a blue jay, a mockingbird, a robin, and a couple I didn't recognize. Oh and a lonely chickadee.
Porch kitty demonstrating her kitty door (and delicate, feline sensibilities about getting her paws damp):
Wednesday, January 20, 2010
NAVC recap
The last week has been an absolute whirlwind of activity. I'm exhausted. It's been a totally different experience when compared with NAVC last year. I came alone in 2009, and while I enjoyed the family time, a conference is a rather lonely experience without friends and/or colleagues.
This year, I was joined by inarguably my 2 closest friends from vet school. Our days began at around 7am and tended to end past 11:00pm. On top of that, one of my internmates was there. We didn't get along well during my internship, but that was partly because an internship is such a hard experience. Now that it's over, I really, really enjoyed her company. Add to that this funny occurrence: I walked into my very first meeting, with over 400 vets, sat down, and realized that 3 seats down was a relief veterinarian from my current town. She pulls ER shifts for us occasionally. I always liked her a lot at work, but I've never seen her much outside of it. She joined our little posse as well (and was in the lab with me). All in all, it was a thoroughly fun, busy experience.
There were lots of great learning opportunities at the conference. I took a great wet lab (Advanced Emergency Procedures). We attended the Foreigner concert on Monday night, as well. Last night was the Sea World shindig sponsored by Schering-Plough. The whole of Sea World was rented out for us last night. The beer and wine was free, the food was free, the games were free, the 2 big coasters (Manta and Kraken) were open, as was Journey to Atlantis (flume ride). There were dolphin and sea lion shows. The finale was the Shamu show (which, while hokey and a little obnoxious due to the loud, cheesy music and video show, was still fantastic).
We slept "late" this morning (i.e. 9am) and then I took them to the airport. I have one more day here, then I too, shall head home. Speaking of home, it has not been without its excitement. My African grey and Senegal got into a big fracas. The grey was (of course!) uninjured. My Sennie wound up having to see the avian vet in our town last night (luckily, a friend AND neighbor). He spent the night at my work, but he is home today and expected to recover fine.
Did I mention how tired I am?
This year, I was joined by inarguably my 2 closest friends from vet school. Our days began at around 7am and tended to end past 11:00pm. On top of that, one of my internmates was there. We didn't get along well during my internship, but that was partly because an internship is such a hard experience. Now that it's over, I really, really enjoyed her company. Add to that this funny occurrence: I walked into my very first meeting, with over 400 vets, sat down, and realized that 3 seats down was a relief veterinarian from my current town. She pulls ER shifts for us occasionally. I always liked her a lot at work, but I've never seen her much outside of it. She joined our little posse as well (and was in the lab with me). All in all, it was a thoroughly fun, busy experience.
There were lots of great learning opportunities at the conference. I took a great wet lab (Advanced Emergency Procedures). We attended the Foreigner concert on Monday night, as well. Last night was the Sea World shindig sponsored by Schering-Plough. The whole of Sea World was rented out for us last night. The beer and wine was free, the food was free, the games were free, the 2 big coasters (Manta and Kraken) were open, as was Journey to Atlantis (flume ride). There were dolphin and sea lion shows. The finale was the Shamu show (which, while hokey and a little obnoxious due to the loud, cheesy music and video show, was still fantastic).
We slept "late" this morning (i.e. 9am) and then I took them to the airport. I have one more day here, then I too, shall head home. Speaking of home, it has not been without its excitement. My African grey and Senegal got into a big fracas. The grey was (of course!) uninjured. My Sennie wound up having to see the avian vet in our town last night (luckily, a friend AND neighbor). He spent the night at my work, but he is home today and expected to recover fine.
Did I mention how tired I am?
Friday, January 15, 2010
If you want a taste
of veterinary student perspective - head over to http://dvm2be.blogspot.com/. Hermit Thrush is a 1st year veterinary student at Cornell in Ithaca, NY. You can also read my back files, although there is a 1 year gap. I've been rather slow in reposting all of my old vet school posts. I'm getting there, I promise.
Thursday, January 14, 2010
Update on : Lessons in bladder control (see bottom)
A 9 month old puppy presented to me on Sunday night around 9pm. She was down-in-the -dumps sick: dehydrated, vomiting, and passing a large amount of very, very bloody diarrhea. She looked like your typical parvo puppy. The parvo test was negative, and the white blood cell count was a whopping 60,000 (normal up to 13,000 or so). I discussed starting aggressive treatment with fluids and antibiotics to the owners (coincidentally, these are the same owners whose cockatoo I treated a month or so ago).
We started treatment, but the puppy continued to deteriorate despite aggressive fluid replacement. I palpated her abdomen again carefully, and I could swear I felt a mass that kept moving - disappearing momentarily and then coming back. After really mulling it over, I decided to call the owners back and tell them that I thought exploratory surgery was warranted. It was a hard call to make. The xrays didn't show an obvious foreign body, but they were UGLY. I had a hunch something was seriously wrong. As a sidenote: one of the things vets hate most is doing a negative exploratory (not finding anything obvious to explain the clinical signs - such as a foreign body or strangulated bowel loop). The owners, despite financial concerns, opted to go for it.
I was not quite prepared for what I found (although I should have been, as what I found is a big differential for bloody diarrhea in a puppy). The intestines were kind of a knot, and there was fibrin in the abdomen. The omentum (membrane that covers and nourishes the guts) was adhered to the big knot in the middle. I gently pulled it out and stared at it, not quite sure what I was looking at. As I teased the omentum away slowly, I finally understood. I was staring at my first GI intussusception.
That big fancy word describes when the intestines become hyper-motile and telescope in on themselves. Essentially, the large intestines try to eat the small intestines. Often, it becomes stuck that way - as this puppy's had - probably a couple of days ago. If it's a fresh intussusception, you can milk the intestines out of themselves and presto majesto finito. In this case, the problem had been present for at least 2 days. I could slide my finger into where the guts telescoped, and feces came back out. There was a hole inside. That meant only one thing: a resection and anastamosis.
I had to cut out the bad part and sew the good ends together. In the small intestines, this isn't hard - they heal great. In this case, however - I had to cut the colon/large intestine. It DOES NOT heal well. You never cut into the colon unless you have no other choice. I had none.
I cut it out, sewed it back together, debated whether it looked healthy, and finally, took a deep breath, tried not to pee on myself in fear, and closed up the dog.
Four days later, she is doing great. No more vomiting, she's eating, wagging her tail, and totally normal. The first 48-72 hours are critical, but I think we can safely say that we're out of the woods now.
That surgery was a huge rush for me. It was my first of that kind, and I was very proud of the way I handled it. 2 hours from start to finish, and my patient is doing GREAT.
Ahh! Sometimes I love my job.
Update: My patient recovered beautifully (this is an old post from September) and to this day, is growing like a weed and healthy as a horse!
We started treatment, but the puppy continued to deteriorate despite aggressive fluid replacement. I palpated her abdomen again carefully, and I could swear I felt a mass that kept moving - disappearing momentarily and then coming back. After really mulling it over, I decided to call the owners back and tell them that I thought exploratory surgery was warranted. It was a hard call to make. The xrays didn't show an obvious foreign body, but they were UGLY. I had a hunch something was seriously wrong. As a sidenote: one of the things vets hate most is doing a negative exploratory (not finding anything obvious to explain the clinical signs - such as a foreign body or strangulated bowel loop). The owners, despite financial concerns, opted to go for it.
I was not quite prepared for what I found (although I should have been, as what I found is a big differential for bloody diarrhea in a puppy). The intestines were kind of a knot, and there was fibrin in the abdomen. The omentum (membrane that covers and nourishes the guts) was adhered to the big knot in the middle. I gently pulled it out and stared at it, not quite sure what I was looking at. As I teased the omentum away slowly, I finally understood. I was staring at my first GI intussusception.
That big fancy word describes when the intestines become hyper-motile and telescope in on themselves. Essentially, the large intestines try to eat the small intestines. Often, it becomes stuck that way - as this puppy's had - probably a couple of days ago. If it's a fresh intussusception, you can milk the intestines out of themselves and presto majesto finito. In this case, the problem had been present for at least 2 days. I could slide my finger into where the guts telescoped, and feces came back out. There was a hole inside. That meant only one thing: a resection and anastamosis.
I had to cut out the bad part and sew the good ends together. In the small intestines, this isn't hard - they heal great. In this case, however - I had to cut the colon/large intestine. It DOES NOT heal well. You never cut into the colon unless you have no other choice. I had none.
I cut it out, sewed it back together, debated whether it looked healthy, and finally, took a deep breath, tried not to pee on myself in fear, and closed up the dog.
Four days later, she is doing great. No more vomiting, she's eating, wagging her tail, and totally normal. The first 48-72 hours are critical, but I think we can safely say that we're out of the woods now.
That surgery was a huge rush for me. It was my first of that kind, and I was very proud of the way I handled it. 2 hours from start to finish, and my patient is doing GREAT.
Ahh! Sometimes I love my job.
Update: My patient recovered beautifully (this is an old post from September) and to this day, is growing like a weed and healthy as a horse!
Mystery and intrigue
Last Tuesday, an owner called and stated that her dog was having seizures, and she was bringing her in.
When the dog came in, the owner was cradling her in his arms, and the dog was trembling terribly. I rushed to get the Valium while my technician gathered information on the case.
The history: no seizures in the past, normal up until that night. Then the dog went outside to use the bathroom. The owners didn't accompany her to the yard, as it was raining. She was outside for a few minutes, came back inside, and started to "seizure."
The "seizuring" had contiued unabated since then. On presentation, the patient's temperature was 108 degrees. Valium did nothing to help control the "seizures." It was only after the first dose that I realized that my patient wasn't seizuring. She was having terrible, generalized muscle tremoring. The difference was obvious once I really looked at my patient. She was aware of us, attempting to look around, but she couldn't walk due to the tremoring.
I discussed with the owner that I strongly suspected a toxin of some sort. I grilled them about anything she could have gotten into ... moldy food being my biggest concern. The owners were adamant that they knew of nothing.
They went home and left the patient in my care. Over the course of the night, I couldn't get the tremoring under control. I resorted to general anesthesia with propofol (yes, the drug that killed MJ). Strongly suspecting toxin, I also pumped her stomach (gastric lavage) and then gave her activated charcoal. That's the black stuff in the drain. It coats the stomach and prevents further absorption of ingesta. What came out of the tube looked and smelled exactly like moldy food.
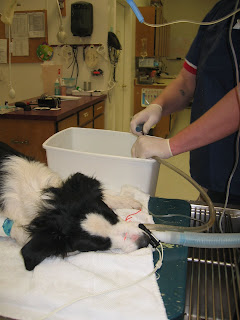

It was around that time that the owner called me back and confessed that her boyfriend had thrown a great deal of moldy food from their fridge into the backyard. Moldy chicken noodle soup, bread, and cheese. They also noted that when the dog came back in the house, it came from the side of the house where the moldy food had been thrown. The tremoring started 30 minutes later, consistent with mycotoxin ingestion. Mycotoxins are mold species that grow on food and can cause severe tremoring in dogs.
Unfortunately, this dog was severely affected, and the owners lacked the funds to treat for the required 2-4 days. She was euthanized later that day at her veterinarian's office.
This case offered an important lesson: what the owner perceives to be occurring and what is actually occurring are not necessarily the same thing. When the dog was presented, I heard what the owners said: seizure and treated accordingly. It was only after assessing my patient that I realized my error. I wish it had made a difference in the outcome for my patient, but sadly, it did not.
When the dog came in, the owner was cradling her in his arms, and the dog was trembling terribly. I rushed to get the Valium while my technician gathered information on the case.
The history: no seizures in the past, normal up until that night. Then the dog went outside to use the bathroom. The owners didn't accompany her to the yard, as it was raining. She was outside for a few minutes, came back inside, and started to "seizure."
The "seizuring" had contiued unabated since then. On presentation, the patient's temperature was 108 degrees. Valium did nothing to help control the "seizures." It was only after the first dose that I realized that my patient wasn't seizuring. She was having terrible, generalized muscle tremoring. The difference was obvious once I really looked at my patient. She was aware of us, attempting to look around, but she couldn't walk due to the tremoring.
I discussed with the owner that I strongly suspected a toxin of some sort. I grilled them about anything she could have gotten into ... moldy food being my biggest concern. The owners were adamant that they knew of nothing.
They went home and left the patient in my care. Over the course of the night, I couldn't get the tremoring under control. I resorted to general anesthesia with propofol (yes, the drug that killed MJ). Strongly suspecting toxin, I also pumped her stomach (gastric lavage) and then gave her activated charcoal. That's the black stuff in the drain. It coats the stomach and prevents further absorption of ingesta. What came out of the tube looked and smelled exactly like moldy food.
It was around that time that the owner called me back and confessed that her boyfriend had thrown a great deal of moldy food from their fridge into the backyard. Moldy chicken noodle soup, bread, and cheese. They also noted that when the dog came back in the house, it came from the side of the house where the moldy food had been thrown. The tremoring started 30 minutes later, consistent with mycotoxin ingestion. Mycotoxins are mold species that grow on food and can cause severe tremoring in dogs.
Unfortunately, this dog was severely affected, and the owners lacked the funds to treat for the required 2-4 days. She was euthanized later that day at her veterinarian's office.
This case offered an important lesson: what the owner perceives to be occurring and what is actually occurring are not necessarily the same thing. When the dog was presented, I heard what the owners said: seizure and treated accordingly. It was only after assessing my patient that I realized my error. I wish it had made a difference in the outcome for my patient, but sadly, it did not.
Wednesday, January 13, 2010
Update on: Here comes mother (see bottom)...
I had my first GDV at the new job (famously known as the mother of all emergencies). It SHOULD have been a breeze. The owners caught it within 15 minutes of the onset of clinical signs (non-productive retching, restlessness, and distended abdomen). It was a Great Dane, so they knew to watch for the signs of a GDV. When I got into the abdomen, the stomach was absolutely healthy and gorgeous - the most lovely pink I've ever seen. No hint of gastric necrosis (death) and no need for any stomach resection. I should have been in and out in about 1 hour, at the most.
Of course, I wasn't. The dog was on prednisone for its skin disease, so she bled and bled and bled and bled (prednisone makes platelets not sticky, just like aspirin, so clots don't readily form). She was 120 pounds, and I had a very hard time decompressing her stomach with the stomach tube. Once it was decompressed, I had a really hard time with the pexy and was not satisfied with the final product at all (tacking it to her body wall so that this wouldn't happen again). Once all that was done, the bleeding in her abdomen just went on and on. I checked everything - liver, mesentery, spleen, kidneys, and couldn't locate a source of bleeding. Everything just oozed. Finally, I lavaged the abdomen with 3 liters of saline, suctioned it out, and closed up the patient. The skin and subcutaneous tissue OOZED AND OOZED. I was terrified she would bleed to death after surgery.
I stared at her obsessively through the night, after my 2.5 hours of surgery. She did well, although her heart rate remained very elevated, despite taking every step to relieve pain, discomfort, and rehydrating her aggressively.
She is back in the ICU tonight for monitoring and continued post-operative care. So far, she is doing very well.
Keep your fingers crossed for her. Being a 9 year old Great Dane is hard enough as it is!
Update: this was originally written in early October. My patient made a full recovery and continues life as a geriatric Great Dane.
Of course, I wasn't. The dog was on prednisone for its skin disease, so she bled and bled and bled and bled (prednisone makes platelets not sticky, just like aspirin, so clots don't readily form). She was 120 pounds, and I had a very hard time decompressing her stomach with the stomach tube. Once it was decompressed, I had a really hard time with the pexy and was not satisfied with the final product at all (tacking it to her body wall so that this wouldn't happen again). Once all that was done, the bleeding in her abdomen just went on and on. I checked everything - liver, mesentery, spleen, kidneys, and couldn't locate a source of bleeding. Everything just oozed. Finally, I lavaged the abdomen with 3 liters of saline, suctioned it out, and closed up the patient. The skin and subcutaneous tissue OOZED AND OOZED. I was terrified she would bleed to death after surgery.
I stared at her obsessively through the night, after my 2.5 hours of surgery. She did well, although her heart rate remained very elevated, despite taking every step to relieve pain, discomfort, and rehydrating her aggressively.
She is back in the ICU tonight for monitoring and continued post-operative care. So far, she is doing very well.
Keep your fingers crossed for her. Being a 9 year old Great Dane is hard enough as it is!
Update: this was originally written in early October. My patient made a full recovery and continues life as a geriatric Great Dane.
Tuesday, January 12, 2010
Update on: Sometimes you lose... (see bottom)
I've been feeling like a rock star surgeon since I arrived at my job. I've had multiple GDVs, c-sections, exploratories, a GI intussusception, and the like. All are alive and kicking!
Last week, I saved a dog that had been hit by a car with a terrible diaphragmatic hernia. Her lungs and heart were being crushed by her spleen, stomach, and liver. Despite her unstable condition, I had to take her to surgery. 3 chest tubes and a diaphragmatic hernia repair later, she is doing great. Despite the odds, she survived!
On Saturday, I took a headless teddy bear out of patient's intestines after she'd been vomiting, lethargic, and depressed for a week. She's doing great, as well.
And finally, my liver lobectomy/giant tumor removal is 2 weeks post op. He is doing great, already feeling good again. His kidney values are improving, he is eating, and his sutures are out. He is recovered.
Those are 3 difficult surgeries. Two of them had guarded to poor prognosis...and yet, they are all alive today. I can look at them and say without a doubt that I saved them.
Yet today puts all of that to the back of my mind. You see, my patient from today is not alive. No, I do not blame myself. Her owners allowed her to roam free, and she was hit by a car. By the time she got to me, her condition was extremely, profoundly terrible. I gave her owners a less than 5% chance for survival, even with surgery. Still, for now, I'm going to sit here and review what I could have done differently for this dog and whether it would have made a difference or not.
She was a large breed puppy (less than a year). She came in after being hit by a car. Her gums were gray-purple. Her systolic blood pressure would not register. She was in profound shock. Her pelvis was broken. She had a pneumothorax. Her condition was grave.
Her owners told me to do whatever it took to save her. Money was not a concern. They plopped down $2100 without batting an eye. So, I went to work. I pumped her full of fluids - crystalloids and colloids. I tapped her chest, eventually placing a chest tube. I was aggressive.
When I checked her initial PCV (packed cell volume), it was 28%. She was losing blood somewhere. When I popped the ultrasound probe on her belly, it was abundantly clear where the blood was going -her belly. My techs wrapped her back legs and abdomen in tight bandages (shock pants). I gave the owners the bad news. We would try to stabilize her, but it was looking like surgery was in her future. When her blood pressure refused to rise above 50 despite massive fluid boluses, and her PCV plummeted to 14 with a total solids of 2.5, I knew we had to cut.
I found the bleeding within 25 minutes of getting into her belly (it took that long to suction out the 2 liters of hemorrhage). One of the liver lobes deep within her abdomen was terribly lacerated. I would either have to perform another lobectomy or find a way to suture the torn liver. Meanwhile, blood continued to pour into the abdomen. We autotransfused her, but the blood just kept pouring out of the liver, as I tried to fix it. My patient's status deteriorated rapidly. Despite the unbelievably low anesthestic level (0.2% sevo!), crystalloids, Hetastarch, and autotransfusion, she could not maintain her blood pressure. I tried everything I could to get to that liver lobe to repair or remove it. I couldn't. At least, I couldn't before she died.
Now, I sit here and question. Should I have tried to get her to the specialty hospital? Should I have hoped the shock pants and pressure wrap would stop the bleeding and held on going to surgery? Did my handling of the liver worsen the damage already done? Would she have bled to death had I waited? Could she have been saved in the first place? Had another ER doctor been there, would she still be alive?
I think I need to rest now. I've been up since 7am this morning, left work well after midnight, and have 2 more nights of work before I get a brief break.
Update: after dealing with this horrific case, I made a plea to our board members for a cautery unit. Cautery units are machines used in surgery. They are great for stopping bleeding, because they cauterize vessels. I'm not sure it would have made a difference in this patient's case, given the extent of injury, but one of the biggest difficulties with this surgery was trying to get the hemorrhage under control. Our board members approved a cautery unit, and it arrived just a few days ago! Yay for improving our standard of care. I am very happy with the hospital where I work, and I am continually pleased by their interest in doing the best we can for our patients!
Last week, I saved a dog that had been hit by a car with a terrible diaphragmatic hernia. Her lungs and heart were being crushed by her spleen, stomach, and liver. Despite her unstable condition, I had to take her to surgery. 3 chest tubes and a diaphragmatic hernia repair later, she is doing great. Despite the odds, she survived!
On Saturday, I took a headless teddy bear out of patient's intestines after she'd been vomiting, lethargic, and depressed for a week. She's doing great, as well.
And finally, my liver lobectomy/giant tumor removal is 2 weeks post op. He is doing great, already feeling good again. His kidney values are improving, he is eating, and his sutures are out. He is recovered.
Those are 3 difficult surgeries. Two of them had guarded to poor prognosis...and yet, they are all alive today. I can look at them and say without a doubt that I saved them.
Yet today puts all of that to the back of my mind. You see, my patient from today is not alive. No, I do not blame myself. Her owners allowed her to roam free, and she was hit by a car. By the time she got to me, her condition was extremely, profoundly terrible. I gave her owners a less than 5% chance for survival, even with surgery. Still, for now, I'm going to sit here and review what I could have done differently for this dog and whether it would have made a difference or not.
She was a large breed puppy (less than a year). She came in after being hit by a car. Her gums were gray-purple. Her systolic blood pressure would not register. She was in profound shock. Her pelvis was broken. She had a pneumothorax. Her condition was grave.
Her owners told me to do whatever it took to save her. Money was not a concern. They plopped down $2100 without batting an eye. So, I went to work. I pumped her full of fluids - crystalloids and colloids. I tapped her chest, eventually placing a chest tube. I was aggressive.
When I checked her initial PCV (packed cell volume), it was 28%. She was losing blood somewhere. When I popped the ultrasound probe on her belly, it was abundantly clear where the blood was going -her belly. My techs wrapped her back legs and abdomen in tight bandages (shock pants). I gave the owners the bad news. We would try to stabilize her, but it was looking like surgery was in her future. When her blood pressure refused to rise above 50 despite massive fluid boluses, and her PCV plummeted to 14 with a total solids of 2.5, I knew we had to cut.
I found the bleeding within 25 minutes of getting into her belly (it took that long to suction out the 2 liters of hemorrhage). One of the liver lobes deep within her abdomen was terribly lacerated. I would either have to perform another lobectomy or find a way to suture the torn liver. Meanwhile, blood continued to pour into the abdomen. We autotransfused her, but the blood just kept pouring out of the liver, as I tried to fix it. My patient's status deteriorated rapidly. Despite the unbelievably low anesthestic level (0.2% sevo!), crystalloids, Hetastarch, and autotransfusion, she could not maintain her blood pressure. I tried everything I could to get to that liver lobe to repair or remove it. I couldn't. At least, I couldn't before she died.
Now, I sit here and question. Should I have tried to get her to the specialty hospital? Should I have hoped the shock pants and pressure wrap would stop the bleeding and held on going to surgery? Did my handling of the liver worsen the damage already done? Would she have bled to death had I waited? Could she have been saved in the first place? Had another ER doctor been there, would she still be alive?
I think I need to rest now. I've been up since 7am this morning, left work well after midnight, and have 2 more nights of work before I get a brief break.
Update: after dealing with this horrific case, I made a plea to our board members for a cautery unit. Cautery units are machines used in surgery. They are great for stopping bleeding, because they cauterize vessels. I'm not sure it would have made a difference in this patient's case, given the extent of injury, but one of the biggest difficulties with this surgery was trying to get the hemorrhage under control. Our board members approved a cautery unit, and it arrived just a few days ago! Yay for improving our standard of care. I am very happy with the hospital where I work, and I am continually pleased by their interest in doing the best we can for our patients!
Monday, January 11, 2010
Sloth: habitual disinclination to exertion; indolence; laziness.
Please tell me that others have become as sloth-like as I have? This cold weather makes me reluctant to leave the house unless absolutely necessary. I spend most of my time curled up in my favorite armchair in front of the fire, reading. The rest of my time is spent watching movies and TV (I've seen the whole, extended version set of Lord of the Rings already) or sleeping. I feel positively lazy. Also, for whatever reason, I cannot get back on a "normal" sleep schedule this time around. I can't figure out why, but my sleep is completely screwed up. Perhaps because I stay home all day? I did venture out last Thursday and meet the local book club at our AMC 24 to see a screening of the Lovely Bones. I met some very nice people and look forward to being a member of a book club, now. I've also been in contact with the local Big Brothers/Big Sisters. I want to volunteer with them, now that I have the time. My husband has had a little since I was in vet school, and he really enjoys it. Lastly, I'm going to sign up for a Spanish class that begins in late January. So, I'm not exactly idle...just this week.
I've delved into the Lord of the Rings books again. This will mark my 3rd time reading them. They're so good, and so detailed, that I feel multiple reads are necessary to fully absorb Tolkein's world.
That about sums up this week. I'm looking forward to NAVC this week enormously! It will certainly keep me busy, and my slothliness (is that a word?) will come to an end.
I've delved into the Lord of the Rings books again. This will mark my 3rd time reading them. They're so good, and so detailed, that I feel multiple reads are necessary to fully absorb Tolkein's world.
That about sums up this week. I'm looking forward to NAVC this week enormously! It will certainly keep me busy, and my slothliness (is that a word?) will come to an end.
Saturday, January 9, 2010
Success story
This is my technician's dog. I removed a 2# nasty, necrotic liver tumor from him in October. At that time, he was anemic, thrombocytopenic (low platelets), his kidney values were elevated, and he was one sick little dog. Now, 3 months out, he is a new dog! Sometimes we do win :) He's dressed up for New Year's Eve, by the way! And yes, despite the dress, it is a HE!



Saturday, January 2, 2010
I'm so excited.
After tomorrow night, I have 17 blissful days off work. YES - SEVENTEEN. I am attending the annual North American Veterinary Conference in Orlando from Jan 16-20. The week prior to that (starting Monday) is my 9 day off stretch. In the interest of not screwing up our carefully organized schedule, I still get my 9 days off, followed by the conference. I'll be staying at my grandparents house about 45 minutes from Orlando. Even better, I'm going with my 2 best friends from vet school. I'm really, really excited to have a big break from work. It won't be good for money making, but at this precise point, I honestly don't care!
Subscribe to:
Posts (Atom)











